Project Description
A Moral Imperative for Healthcare Professionals

When conclusive studies found that smoking caused cancer, many physicians went from being smokers to becoming “leaders by example” in the AMA’s 1972 War on Cancer (AMA Website, May 2022). Today, healthcare workers should be leading the War on Climate Change by reducing greenhouse gas emissions caused by hospitals, surgical centers, and the rest of the health sector – particularly those that come from the supply chain.
If the worldwide health sector was a country, it would be the fifth-largest emitter of greenhouse gas emissions, accounting for almost 5% of all such emissions (HCWH, September 2019).
Climate change is a public health issue that threatens all of us. As water and air pollution increase, so do deadly chronic respiratory diseases (European Respiratory Review, 2014). Rising temperatures due to climate change lead to increased ground-level ozone, which cause airway inflammation and damages lung tissue (Multidisciplinary Respiratory Medicine, 2013). The fact that hospitals are a leading cause of climate change producing emissions should serve as a call to action to all healthcare workers to reduce waste and lower emissions.
A closer look finds that over 80% of greenhouse gas emissions generated by the health sector come from the supply chain (known as “Scope 3” emissions) (Health Affairs, 2020).

Reprocessing SUDs already creates over 3,300 green jobs. If all U.S. hospitals reprocessed all of the FDA-cleared devices, thousands more jobs would be created.
Urgent action is needed, and governments are taking notice. Over forty countries have committed to reducing greenhouse gas emissions from the healthcare sector, including the United States (The New York Times, November 2021).
Given the impact of the sector’s environmental footprint on global health, government-run and government-reimbursed healthcare facilities have a moral responsibility to pursue initiatives that not only identify sources of greenhouse gas emissions from the supply chain, but also find lower-emission alternatives.
Well-intentioned concerns over infection control have further contributed to a “take-make-waste” culture emblematic of our linear healthcare economy. The shift to disposable products has contributed to a mountain of waste generated by hospitals.
Green healthcare advocacy organizations are advocating for less linear, and more circular thinking to reduce the health sector’s greenhouse gas emissions. Some are calling for hospitals to stop throwing away every device after one use while encouraging the use of commercially reprocessed “single-use” devices (SUDs) (HCWH, March 2021).
“Single-Use” Device Reprocessing Provides a Proven Circular Economy Solution

Today, over 300 types of “single-use” devices have been registered and cleared by FDA for reprocessing, deemed “substantially equivalent” to the original device, with no associated additional safety risk.
Over 20 years ago, the FDA reviewed the practice of SUD reuse and created a regulated pathway to assure that reprocessed SUDs met the same regulatory standards as original devices. The unnecessary and wasteful single use of hundreds of products costs health systems (and in the case of the VA, DoD, and CMS-reimbursed hospitals, the taxpayers) hundreds of millions, if not billions, of dollars per year, and simultaneously drives up needless greenhouse gas emissions.
The National Academy of Medicine finds FDA regulated reprocessing to be a key strategy for hospitals to reduce carbon emissions. So too does the Agency for Healthcare Research and Quality, part of the U.S. Department of Health and Human Services. The United Kingdom’s National Health Service (NHS) also advocates for the use of “remanufactured” devices (as they are called in Europe) to reduce greenhouse gas emissions.
NHS, which has committed to reduce greenhouse gas emissions by 80% by 2050, has already implemented an aggressive program that seeks to remanufacture and reuse up to 50% of single-use devices. At right is the NHS guidance and prioritization for reducing emissions and waste with reprocessing coming in as the third-highest priority. 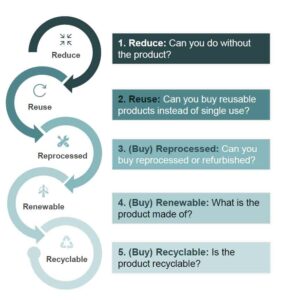
Use of FDA-cleared reprocessed SUDs drives a circular solution that immediately helps to reduce greenhouse gas emissions from the healthcare supply chain, improves supply chain resiliency, and reduces healthcare costs. Circular solutions fuel a circular economy – one based on more sustainable practices of using products until their true end of life is reached.
Thousands of hospitals already use at least some reprocessed SUDs. Because reprocessed SUDs cost 25 to 40% less than using an original device, hospitals realize substantial savings they can use to pay for environmental improvements while adding capacity for better patient care.
 Although the companies that specialize in reprocessing these devices reprocessed over thirty-six million such devices and returned them to over 9,400 hospitals worldwide in 2024 alone, AMDR data finds that only a tiny fraction of FDA-cleared (or CE marked in the EU) SUDs that could legally and safely be reprocessed, are in fact reprocessed.
Although the companies that specialize in reprocessing these devices reprocessed over thirty-six million such devices and returned them to over 9,400 hospitals worldwide in 2024 alone, AMDR data finds that only a tiny fraction of FDA-cleared (or CE marked in the EU) SUDs that could legally and safely be reprocessed, are in fact reprocessed.
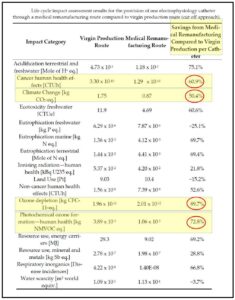
More recently, researchers conducted and published a well-designed life cycle assessment (LCA) of one such “reprocessed” device (an electrophysiology catheter) and found it to reduce ozone depleting emissions by nearly 90%, and climate change-specific emissions by over 50% compared with using an original device (Sustainability, 2021). LCAs of other commonly found single-use medical devices are finding similar emission reductions. We update a bibliography of these and related studies.
While all “America’s Best Hospitals,” as listed by U.S. News & World Report, are realizing the significant benefits of using reprocessed devices, not all are reprocessing to their potential.
COVID provided a wakeup call on the waste and emissions associated with our disposable healthcare economy. The pandemic generated tons of additional medical waste as clinicians dispose of personal protective equipment (PPE) and ancillary medical devices used on COVID patients (The Verge, March 2020). While PPE is not FDA-cleared for reprocessing, the additional costs and waste incurred for PPE, along with the cost to dispose of it, accentuate the need to reprocess those items we can convert from waste to hospital assets through their reuse.
